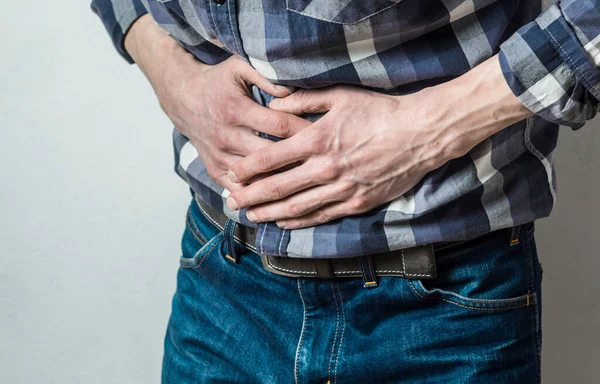
This symptom could be easily dismissed as just a stomach ache or indigestion. Aching Pain on One Side: Could it be Fatty Liver Disease?
Have you ever experienced a dull, nagging pain on one side of your body, particularly your upper right abdomen? While this discomfort can arise from various sources, it’s crucial to consider the possibility of fatty liver disease. While often silent in its early stages, this increasingly common condition can manifest through subtle signals, and early detection is key to preventing its progression.
What is Fatty Liver Disease?
Fatty liver disease is a broad term encompassing a spectrum of conditions characterized by the accumulation of excess fat in the liver. This buildup can impair the liver’s ability to function properly, leading to a range of health problems if left untreated.
There are two main types of fatty liver disease:
- Non-alcoholic fatty liver disease (NAFLD): The most common type, accounting for about 80% of cases. It is not caused by excessive alcohol consumption.
- Non-alcoholic steatohepatitis (NASH): A more severe form of NAFLD characterized by inflammation and liver cell damage. If left unchecked, NASH can progress to cirrhosis, a serious condition with scarring and irreversible liver damage.
The Silent Threat: Early Symptoms of Fatty Liver Disease
Unfortunately, fatty liver disease often progresses silently, with many individuals experiencing no symptoms in the early stages. However, some people may notice:
- A dull, aching pain in the upper right abdomen (under the ribs): This is the most common symptom, but it can be easily mistaken for other conditions like indigestion or muscle strain.
- Fatigue: Feeling tired and run down is a frequent complaint among people with fatty liver disease.
- Loss of appetite: This can be due to the liver’s impaired ability to process nutrients.
- Nausea and vomiting: These symptoms can occur if the fatty liver puts pressure on other organs in the abdomen.
- Weight loss: This is less common than weight gain, but can occur in some cases.
Study Spotlight: Recognizing the Signs Early
A recent study published in the Journal of Hepatology by the National Health Service (NHS) in the UK sheds light on the importance of early symptom recognition. The study followed over 5,000 individuals with NAFLD and found that those who experienced early symptoms, particularly fatigue and abdominal pain, were more likely to develop more advanced stages of the disease, including cirrhosis. This emphasizes the need to be aware of these seemingly minor symptoms and seek medical advice if they persist.
However, there are many other symptoms including:
- Tiredness and weakness
- Loss of appetite
- Weight loss and muscle wasting
- Feeling sick (nausea) and vomiting
- Tenderness or pain around the liver area
- Tiny red lines (blood capillaries) on the skin above waist level
- Very itchy skin
- A tendency to bleed and bruise more easily, such as frequent nosebleeds or bleeding gums
- Hair loss
- Fever and shivering attacks
- Swelling in the legs, ankles and feet due to a build-up of fluid (oedema)
- Swelling in your abdomen (tummy), due to a build-up of fluid known as ascites (severe cases can make you look heavily pregnant).
“You may also notice changes in your personality, problems sleeping (insomnia), memory loss, confusion and difficulty concentrating,” NHS Inform adds.
If you experience any symptoms of fatty liver disease you should speak to your doctor.
Beyond the Ache: Understanding the Causes of Fatty Liver Disease
While the exact cause of fatty liver disease is not fully understood, several factors contribute to its development:
- Obesity: Carrying excess weight, especially around the abdomen, is a major risk factor for NAFLD. Studies suggest that individuals with a body mass index (BMI) of 30 or higher are significantly more likely to develop the condition.
- Insulin resistance: This occurs when the body’s cells become less responsive to the hormone insulin, which regulates blood sugar levels. Insulin resistance is a hallmark of type 2 diabetes and a major contributor to NAFLD.
- High cholesterol: Elevated levels of bad cholesterol (LDL) and low levels of good cholesterol (HDL) can increase the risk of fatty liver disease.
- Certain medications: Some medications, such as corticosteroids and certain cholesterol-lowering drugs, can have side effects that contribute to fatty liver.
- Excessive alcohol consumption: While not the primary cause of NAFLD, heavy alcohol consumption can further damage the liver in individuals with pre-existing fatty liver disease.
- Other medical conditions: Polycystic ovary syndrome (PCOS), sleep apnea, and hypothyroidism can also increase the risk of fatty liver disease.
Diagnosing and Treating the Aching Truth
Early diagnosis and intervention are crucial in managing fatty liver disease and preventing its progression. The first step usually involves a physical examination and a discussion of your medical history and symptoms. Your doctor may also recommend:
- Blood tests: These can assess liver function, check for inflammation, and identify other underlying conditions.
- Imaging scans: Ultrasound, CT scan, or MRI can provide detailed images of the liver and assess fat accumulation and damage.
Treatment focuses on addressing the underlying cause and slowing the progression of the disease. This typically involves:
- Lifestyle changes: These are the cornerstone of treatment, including maintaining a healthy weight through diet and exercise, managing insulin resistance, and reducing alcohol consumption.
- Medications: In some cases, your doctor may prescribe medications to manage cholesterol levels, reduce inflammation, or improve insulin sensitivity.
- Liver transplantation: In severe cases of cirrhosis, liver transplantation may be necessary.
Preventing the Aches and Beyond: A Proactive Approach
The good news is that fatty liver disease is often reversible with lifestyle changes. Here are some key steps you can take to reduce your risk and promote liver health:
Maintaining a Healthy Weight: Your First Line of Defense
Aim for a healthy Body Mass Index (BMI) within the range of 18.5-24.9. Even modest weight loss (5-10%) can significantly improve liver health and reduce fat accumulation. Consult a registered dietitian or healthcare professional for personalized guidance on healthy weight management strategies.
Embrace a Balanced Diet: Nourishing Your Liver
Nutrient-rich foods contribute to optimal liver function and protection. Prioritize:
- Fruits and vegetables: Packed with antioxidants and fiber, these promote detoxification and reduce inflammation. Choose a variety of colors for diverse nutrient benefits.
- Whole grains: Opt for brown rice, quinoa, oats, and whole-wheat bread for sustained energy and improved insulin sensitivity.
- Lean protein: Sources like fish, chicken, beans, and lentils provide essential amino acids for repair and rebuilding.
- Healthy fats: Include monounsaturated and polyunsaturated fats like olive oil, avocados, and nuts for cell health and inflammation control.
- Limit saturated and trans fats: Found in processed foods, fried dishes, and red meats, these contribute to fat accumulation in the liver.
- Minimize added sugars and refined carbohydrates: These can worsen insulin resistance and promote fat storage. Opt for natural sweeteners and whole grains over sugary drinks and white bread.
Move Your Body: Exercise is Your Liver’s Friend
Regular physical activity plays a crucial role in managing weight and improving insulin sensitivity. Aim for at least 150 minutes of moderate-intensity exercise or 75 minutes of vigorous-intensity exercise per week. Incorporate activities you enjoy, such as brisk walking, swimming, cycling, dancing, or team sports.
Manage Stress: Find Your Calm
Chronic stress can exacerbate inflammation and negatively impact liver health. Explore stress-management techniques like yoga, meditation, deep breathing exercises, spending time in nature, or engaging in hobbies you find relaxing.
Prioritize Sleep: Restoring Your Body and Mind
Aim for 7-8 hours of quality sleep each night. Adequate sleep is essential for overall health, including liver function. Establish a regular sleep schedule, create a relaxing bedtime routine, and avoid screen time before bed.
Limit Alcohol Consumption: Moderation is Key
Excessive alcohol consumption is a major contributor to fatty liver disease and liver damage. If you choose to drink, do so in moderation. The current guidelines recommend no more than two drinks per day for men and one drink per day for women.
Talk to Your Doctor: Early Detection is Vital
Schedule regular checkups with your doctor, especially if you have any risk factors for fatty liver disease. Discuss your concerns and any symptoms you experience. Early diagnosis and intervention significantly improve the prognosis and prevent complications.
Remember: Fatty liver disease is a manageable condition, but it requires awareness and proactive action. By prioritizing a healthy lifestyle, including balanced diet, regular exercise, stress management, and adequate sleep, you can empower your liver and achieve optimal health.
Read Also | How Probiotics and Prebiotics in Fermented Foods Impact Mental Health
Additional Resources:
- National Institute of Diabetes and Digestive and Kidney Diseases: https://www.ncbi.nlm.nih.gov/books/NBK541033/
- American Liver Foundation: https://liverfoundation.org/
- British Liver Trust: https://britishlivertrust.org.uk/