These 25 Best High-Protein, Low-Fat Foods You Can Eat – Weight loss, muscle gain, and overall health are top priorities for many, and high-protein, low-fat foods offer a winning combination. These foods provide the building blocks for strong muscles, the fuel to keep you energized, and the satisfaction to keep cravings at bay—all while keeping unwanted fat in check.
Protein is an essential macronutrient for building and repairing tissues, promoting satiety, and boosting immune health. And while healthy fats deserve a place in a balanced diet, because this macronutrient is calorically dense, eating fat in moderation is key to weight maintenance or loss.
Eating high-protein, low-fat foods from whole-food sources can not only support healthy weight management, but it can also improve your overall health and well-being. These whole-food protein sources are rich in other essential nutrients like vitamins, minerals, and antioxidants, making them a no-brainer addition to your diet.
So, if you’re looking to boost your protein intake while keeping fat in check, read on for the 25 best high-protein, low-fat foods that can easily fit into your diet and help you achieve your health goals. Adding these to your daily diet or weekly meal rotation will help you shed extra pounds and keep them off.
Edamame

Serving size: 100 grams
Calories: 121
Protein: 12 grams
Fat: 5 grams
Destini Moody, RDN, CSSD, LD, a registered dietitian and sports dietitian with Garage Gym Reviews, tells Eat This, Not That!, “Edamame is one of the rare sources of plant protein that is a complete protein source. That means it contains all the essential amino acids the body needs, which is particularly important for muscle growth and maintenance.” Edamame also contains isoflavones that are associated with antioxidant properties that can boost overall health.
Beef Jerky

Serving size: 28 grams
Calories: 60
Protein: 10 grams
Fat: 2 grams
“Beef jerky is made by removing most of the fat content from the beef during the drying process, making it a convenient protein-rich snack with relatively low-fat content,” explains Gianna Masi, CPT, RDN, a certified personal trainer and registered dietitian with Barbend. Look for beef jerky products low in fat and sodium when possible.
Lentils

Serving size: 1 cup
Calories: 116
Protein: 9 grams
Fat: 0 grams
Lentils are a plant-based protein powerhouse high in fiber, iron, and folate. “Lentils are in the same category as beans, which means they’re a starchy vegetable and a carb source,” says Moody. “However, they’re also an impressive source of protein, making them an excellent addition to meals like salads and soups for a low-fat protein boost.”
Turkey Jerky

Serving size: 28 grams
Calories: 60
Protein: 6 grams
Fat: 0 grams
Turkey jerky is lower in fat than beef jerky but still provides a savory and satisfying snack to help keep you full between meals. “Turkey jerky provides protein with minimal fat, making it a suitable choice for those looking to reduce their fat intake while enjoying a savory and portable snack,” says Masi.
Shrimp

Serving size: 3 ounces (85 grams)
Calories: 84
Protein: 20 grams
Fat: 0 grams
Shrimp is a low-fat protein source rich in omega-3 fatty acids and selenium, which are crucial for heart health and immune function. Moody says, “Shrimp is one of the leanest sources of animal protein you can get, meaning it has one of the lowest fat contents relative to protein content, making it a fantastic choice for pescatarians and non-red meat eaters.”
Top Sirloin

Serving size: 100 grams
Calories: 205
Protein: 21 grams
Fat: 13 grams
“Top sirloin offers a decent amount of protein while being leaner compared to some other cuts, making it a suitable choice for those seeking a balance between flavor and lower fat content,” states Masi. Additionally, red meat cuts like top sirloin are excellent sources of iron, vitamin B12, and zinc, which support good overall health.
Pork Tenderloin
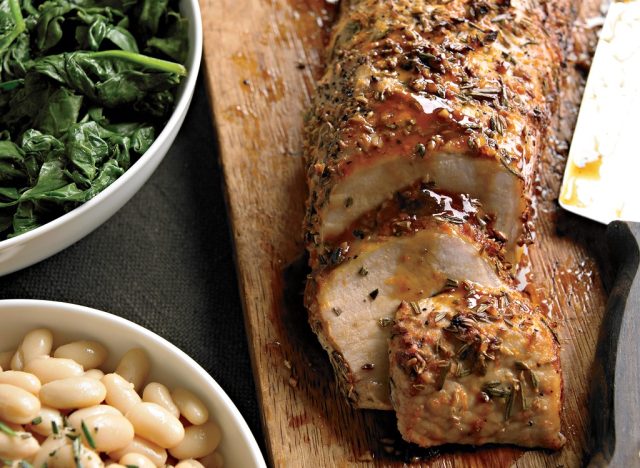
Serving size: 3 ounces (85 grams)
Calories: 122
Protein: 22 grams
Fat: 3 grams
Pork tenderloin is another lean meat option that delivers an array of vitamins and minerals like thiamine, niacin, and selenium. “Given pork’s bad reputation, it may shock most people to hear that pork tenderloin has less fat than chicken breast. This is because it comes from the pig’s backside, which is the less fatty portion,” says Moody.
Cod

Serving size: 100 grams
Calories: 71
Protein: 15 grams
Fat: 0 grams
Cod is a mild-flavored fish that’s low in fat, high in protein, and contains a good amount of omega-3 fatty acids to support heart and brain health. Masi tells us, “Cod is a particularly protein-rich and lean choice among seafood, making it a heart-healthy option for those aiming to reduce fat intake.”
Tilapia

Serving size: 1 fillet (87 grams)
Calories: 111
Protein: 23 grams
Fat: 2 grams
Tilapia is another lean fish option high in protein and low in calories. “Due to tilapia’s mild flavor, it absorbs seasonings well, so you can make it fit nearly any flavor profile,” says Moody.
Flounder

Serving size: 100 grams
Calories: 88
Protein: 19 grams
Fat: 1 gram
“Flounder is a lean fish with a mild flavor. It’s low in fat, making it a good choice for those looking to maintain a healthy diet without compromising on taste,” says Masi. Flounder is also a good source of vitamins and minerals, such as vitamin B12, niacin, and phosphorus.
Tuna

Serving size: 3 ounces (85 grams),
Calories: 132
Protein: 28 grams
Fat: 1 gram
Tuna is a solid protein option, offering nearly 30 grams per 3-ounce serving and only 1 gram of fat. “Tuna is fantastic not only because it is budget-friendly, but you don’t have to worry about it going bad in the fridge before you have a chance to cook that fish dinner. That’s why many dietitians recommend keeping tuna in the pantry as a staple in case you need a solid protein for a meal in a pinch,” explains Moody.
Deli Meat (Chicken or Turkey)

Serving size: 100 grams
Calories: 107
Protein: 23 grams
Fat: 2 grams
Deli meat, especially chicken or turkey, is a convenient protein addition to sandwiches and salads. However, look for cuts of deli meat that are low in sodium and nitrate-free if possible to keep it on the healthy side.
Masi: Deli meats like chicken or turkey can be low-fat options, especially if you choose lean cuts,” Masi explains. “Choose options labeled as “lean” or “low-fat” to ensure a healthier choice for sandwiches or salads.”
Cottage Cheese

Serving size: 100 grams
Calories: 98
Protein: 11 grams
Fat: 4 grams
Cottage cheese is a versatile and underrated protein source. It’s also an excellent calcium source that can be enjoyed on its own or added to smoothies, salads, or baked goods. “You can enjoy cottage cheese savory or sweet by blending it with some spices to make it a dip for chips or add fresh fruit for a sweet post-workout snack,” says Moody. “Just try to get low-fat versions, as more fat means less protein by weight.”
Turkey Bacon

Serving size: 100 grams
Calories: 107
Protein: 16 grams
Fat: 2 grams
Turkey bacon makes for a healthy swap for regular bacon since it’s lower in saturated fat. However, while turkey bacon still contains some fat, Masi says it is generally lower in saturated fat and can be a flavorful option for those looking to reduce their overall fat intake.
Non-Fat Greek Yogurt

Serving size: 100 grams
Calories: 59
Protein: 10 grams
Fat: 0 grams
Non-fat Greek yogurt is a creamy and delicious high-protein snack that can boost your gut health with its rich probiotic content. To incorporate non-fat Greek yogurt into your diet, Moody suggests using a plain version as a sour cream substitute to get more protein with less saturated fat and fewer calories.
Chicken Sausage

Serving size: 100 grams
Calories: 146
Protein: 19 grams
Fat: 4 grams
“Chicken sausage can be a lower-fat option than pork sausage,” says Masi. “Many brands offer leaner chicken sausage, such as Bilinski or Alfresco.” For a healthier option, look for chicken sausage products that are lower in sodium and fat.
Whey Protein Powder

Serving size: 25 grams
Calories: 90
Protein: 20 grams
Fat: 1 grams
You’d be hard-pressed to find a more convenient high-protein, low-fat option than whey protein powder. Mix it with water or milk as a quick post-workout meal or snack, and you’re good to go.
“Nutrition facts vary widely depending on your chosen brand, but the best protein powder brands have at least 20 grams of protein per scoop and as little fat and carbs as possible,” says Moody. “This is beneficial because protein powder is supposed to help supplement your protein intake without adding extra calories from macronutrients you don’t need.”
Seitan

Serving size: 100 grams
Calories: 82
Protein: 12 grams
Fat: 0 grams
Seitan (“wheat meat”) is a vegan-friendly plant-based protein source made from gluten. Its versatility makes it a superb meat substitute in a variety of dishes. “Seitan is naturally low in fat and can be a versatile option for those following vegetarian or vegan diets while aiming to keep fat intake in check,” says Masi.
Tofu

Serving size: 100 grams
Calories: 76
Protein: 8 grams
Fat: 5 grams
Tofu is a soy-based complete protein source high in iron and calcium. “For those who don’t eat animal products, tofu can be a lifesaver,” says Moody. “It’s slightly higher in fat than other products on this list but is still low-calorie and nutrient-dense. It’s also a versatile food that can be seasoned and prepared to taste like other foods while containing all essential amino acids.”
Tempeh

Serving size: 100 grams
Calories: 190
Protein: 21 grams
Fat: 5 grams
Tempeh is another soy-based protein source that’s low in fat. It’s made from fermented soybeans, which can make it easier to digest and support gut health. “Tempeh is a fermented soy product that provides a good source of plant-based protein,” says Masi. “While it contains some fat, it’s generally considered a nutrient-dense, low-fat option for those looking to incorporate more plant-based proteins into their diet.”
Bison

Serving size: 100 grams
Calories: 146
Protein: 20 grams
Fat: 7 grams
“Like most game meats, including deer, elk, and venison, bison is a red meat much leaner than beef,” says Moody. “That’s because wild meat isn’t usually subject to factory farms that leave animals sedentary and grain fed, both of which increase the fat content in their meat.” Bison is a lean meat that’s healthier for meat lovers since it’s lower in fat and calories than beef.
Quinoa

Serving size: 42 grams
Calories: 140
Protein: 6 grams
Fat: 2 grams
Quinoa is a complete protein source containing all nine essential amino acids. It’s also high in fiber and other essential nutrients. Masi tells us, “Quinoa is a whole grain that’s low in fat and high in protein. It also offers a good amount of fiber and various vitamins and minerals, making it a nutritious and low-fat option for a base in salads, bowls, or as a side dish.”
Egg Whites

Serving size: 100 grams
Calories: 52
Protein: 11 grams
Fat: 0 grams
“If you want to reduce your overall fat intake while getting one of the highest-quality protein sources available, egg whites are the food for you,” says Moody. “Egg protein is highly digestible and one of the richest dietary sources of essential amino acids. Also, without the yolk attached, there’s virtually no fat.” Egg whites are a versatile food that go well in omelets, scrambles, and baking for a solid protein boost without the fat content.
Chickpeas

Serving size: 1/2 cup
Calories: 120
Protein: 6 grams
Fat: 2 grams
Chickpeas, or garbanzo beans, are versatile legumes high in fiber and plant protein but have little fat. “Chickpeas are a low-fat legume that provides a good source of protein, fiber, and various nutrients. They’re versatile and can be included in salads, bowls, or as a snack, offering a satisfying and nutritious option for those aiming to limit fat intake,” says Masi.
Soy Milk

Serving size: 1 cup
Calories: 131
Protein: 8 grams
Fat: 4 grams
This dairy-free alternative is an excellent protein source often fortified with calcium and vitamin D. “A great protein source for vegans and those with lactose intolerance, soy milk is my plant-based milk of choice,” states Moody. “The reason soy milk is a good milk substitute is that it has a macronutrient and amino acid profile similar to cow’s milk when compared to other plant milk beverages.”







